 If the OP is due to an inhalational or medication exposure, removal of the inciting agent is essential. When a diagnosis of secondary OP is made, prognosis and response to corticosteroids correlate more closely with the specific etiology. Specific causes for secondary organizing pneumonia (OP) include infections, drug and environmental exposures, and connective tissue diseases (particularly rheumatoid arthritis and polymyositis/dermatomyositis/anti-synthetase syndrome). A key point in the evaluation of organizing pneumonia is that the clinician must search carefully for an underlying etiology that might lead to the same clinical and pathological features of COP. However, the majority of cases in which organizing pneumonia is found are non-cryptogenic. Figure 4.Ĭhest radiograph in cryptogenic organizing pneumonia.ĬOP is the idiopathic form of this disease. 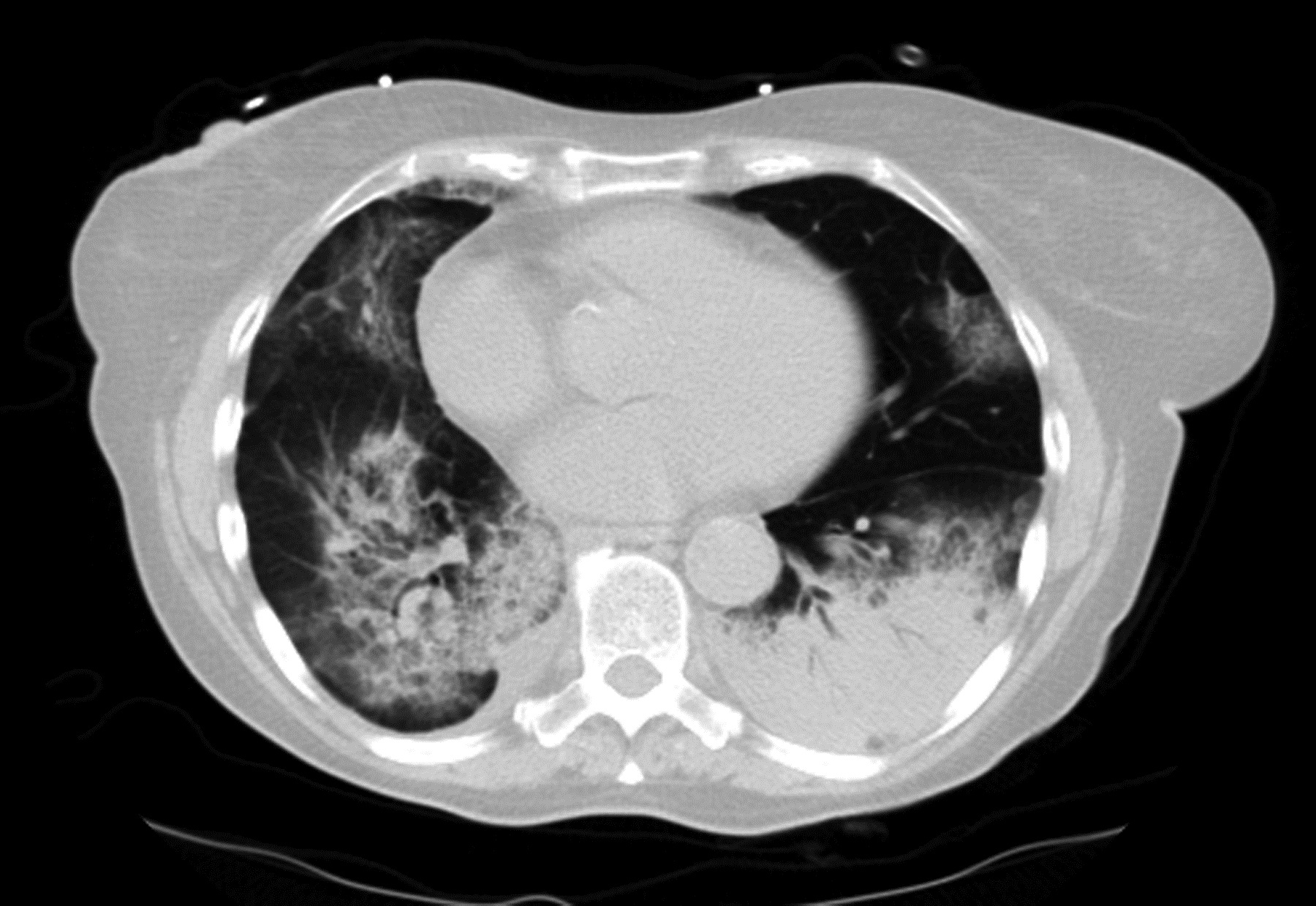
Figure 3.Ĭryptogenic organizing pneumonia on HRCT. Relapse of disease with steroid taper is common with the initial course of therapy, however patients tend to respond to retreatment with corticosteroids, and slower tapers may be required.Ĭryptogenic organizing pneumonia on HRCT. Treatment with corticosteroids leads to dramatic clinical improvement in the majority of cases. Diagnosis is confirmed by the demonstration of organizing pneumonia on surgical lung biopsy. Typical radiographic features include peripheral or peribronchovascular patchy, often migratory ground-glass opacities and consolidation on CXR or high-resolution chest CT (Figure 1) (Figure 2) (Figure 3) (Figure 4). Patients are often initially diagnosed with community acquired pneumonia, and it is only when there is a lack of response or worsening with antibiotic therapy that the possibility of COP is raised. 
The typical clinical features of COP are subacute onset over weeks to months of a mild, flu-like illness characterized by cough, fever, malaise, and progressive dyspnea, and frequently accompanied by weight loss. That’s my humble opinion and two cents worth.Cryptogenic organizing pneumonia (COP) (formerly known as bronchiolitis obliterans organizing pneumonia or BOOP) is a form of idiopathic interstitial pneumonia. The inflammation has to go somewhere, so it goes to the lungs. I know MC is an autoimmune disorder where your gut is inflamed and irritated. I think life-long silent Celiac Disease and Microscopic Colitis caused BOOP PNEUMONIA. I informed my pulmonogist and that’s what he uses now. You can cure BOOP with Macrolides – clarithromycin and azithromycin, and bypass the deadly steroids. HORRORS! I did research and ordered the book – “BOOP: You’re The Boss”. 
The doctor did an X-ray and biopsy of my lungs and I witnessed my lungs were pure White, INFLAMMATION!!! I found out that Gut and Lung tissue are similar or the same. It’s Idiopathic or doctors don’t know what causes BOOP. Okay! Then I was diagnosed with BOOP Pneumonia. Then I was diagnosed with Microscopic Colitis, (MC). I’ve had life-long silent Celiac Disease and didn’t know it. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
